20 September 2022: Clinical Research
Intensive Care Residents’ Views Regarding Ethical Issues and Practices
Şükran Sevimli1ABCDEF*, Arzu Esen Tekeli2ABCDEFDOI: 10.12659/MSM.937357
Med Sci Monit 2022; 28:e937357
Abstract
BACKGROUND: This study sought to understand the ethical issues encountered by medical residents during their residencies, evaluate the solutions proffered by them, and present their suggestions.
MATERIAL AND METHODS: A survey consisting of 32 questions, including demographic information, was developed and distributed to Intensive Care Unit (ICU) residents from December 2020 to January 2021. A total of 53 completed questionnaires were submitted to the researchers. The data were analyzed using SPSS software version 26.0.
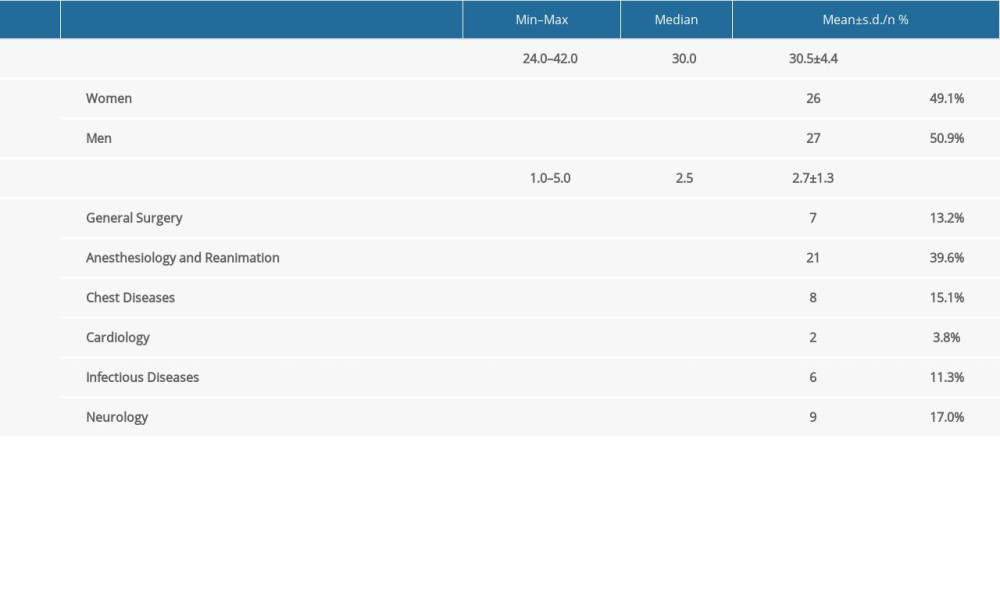
RESULTS: Of the participating residents who returned completed forms, 50.9% were male and 49.1% were female, with an overall mean age of 30.5±4.4 years. Most residents’ views on ethical issues concerned themselves, the clinic, and patients/patient relatives. Responses showed a number of commonalities with the views of ICU physicians in other countries. Suggestions for resolving ethical issues solutions included instruction in medical ethics for all staff, increasing and strengthening pathways of communication both inside and outside of the clinics, regular inventory of medical supplies and assessment of equipment to prevent a shortage of resources, and the establishment of a hospital ethics committee.
CONCLUSIONS: As numerous and varied ethical issues were encountered in the participating ICUs, we propose the following: preparation of an ICU-specific guide for resolving ethical problems, clarification of rules based on legal regulations, determining a hierarchy of responsibilities, and ethics courses for all ICU staff. In addition, hospital managers should support ICU services from both a legal and ethical standpoint.
Keywords: Bioethics, Ethics, Intensive Care Units, Adult, Critical Care, Ethics, Medical, Female, Humans, Internship and Residency, Male, Physicians, Surveys and Questionnaires
Background
The Intensive Care Unit (ICU) is a complex organization of trained healthcare professionals and advanced technical equipment used in the treatment of critically ill patients. Intensive care physicians routinely encounter ethically complex situations, as they have to decide how to treat or prolong the lives of their patients, incorporating the attitudes and expectations of the patient or their relatives, together with medical and ethical values [1]. According to the literature, the main ethical issues arising in ICUs involve patient admission and discharge decisions, which treatments are in the patient’s best interests [2], conflicts over treatment modality or futile treatment, and decision-making at the end of life [3]. The conflicts arising from the ethical issues in question usually occur among the medical teams, the patients/surrogates, or between the patient’s care goals and patient surrogates.
Ethical issues in the ICU should be carefully evaluated by examining all of the relevant parameters and incorporating all of the stakeholders in the ICU. However, making fast (and correct) decisions in accordance with ethical values is an absolute necessity in ICU units [4]. Nowadays, the general public is better informed regarding patient rights and related ethical issues (eg, beneficence, non-maleficence, autonomy, and justice) in health care, and therefore has higher expectations of medical care. In the ICU, patients/patient relatives and healthcare professionals need to focus on the same problems, requiring quick and correct decisions, in what is an extremely stressful climate. Certain ethical issues inevitably arise as a result of differential expectations and of course knowledge with respect to solving the patient’s health problems. Healthcare professionals may vary in their approaches to care or treatment recommendations; even greater differences may be observed between healthcare professionals and patients/surrogates in terms of their attitudes towards and expectations of patient care. For this reason, minimizing these differences and meeting on common ground, based on shared ethical values is of primary importance in choosing and applying the most appropriate course of treatment for the patient.
Numerous studies concerning ethical issues specific to the ICU have been carried out with the participation of nurses or doctors. However, in hospitals that also provide medical resident education, resident physicians are also among the stakeholders in the ICU. Therefore, obtaining the opinions of every healthcare professional, including medical residents, working in the ICU will contribute to both intra- and inter-department cooperation and enable us to better evaluate ICU ethical issues from different perspectives. Medical residents occupy a different position in the hierarchy as they are neither medical students nor fully authorized physicians in the department; nonetheless, they closely follow, observe, and are aware of the many value-based clinical issues, and are even affected by coming face to face with these issues, although they are not at liberty to intervene in these problems [5]. To date, however, there have been few studies examining ethical issues that incorporate the viewpoints of medical residents.
This study aimed to provide answers to the following 2 questions: What are the ethical issues that arise in the ICU, according to the medical residents? And what are their suggestions to solve these problems?
Material and Methods
STATISTICAL ANALYSES:
The data were analyzed using SPSS 26.0 software. For descriptive statistics of the data, the mean, standard deviation, median, lowest and highest frequency, and ratio values were used. The distribution of variables was determined using the Kolmogorov-Smirnov (KS) test and the Mann-Whitney U-test was used to analyze quantitative independent variables. The Cronbach’s alpha coefficient for the total scale was.837. A value of
Results
DOMAIN 1. FREQUENCY AND ROOT CAUSES OF ETHICAL ISSUES; PATIENT ADMISSION, TREATMENT, AND DISCHARGE:
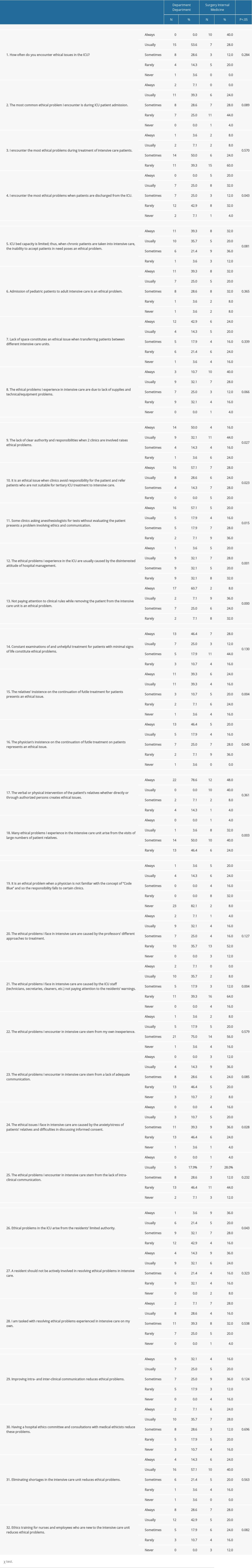
Most residents responded that they sometimes or rarely encounter ethical issues in the ICU, usually during admission and less often during treatment; the internal medicine and surgery residents were in overall agreement on this point (
DOMAIN 2. SCARCITY OF RESOURCES (BEDS, MEDICAL SUPPLIES, ADVANCED TECHNOLOGY):
A majority of the respondents agreed that ethical problems arise in cases of long-term patients, pediatric patients moving into adult intensive care, and patients being transferred between intensive care units for various reasons, as ICUs may not be able to accommodate all patients who require such care due to medical and/or technological deficiencies in the ICU. The responses of the 2 groups did not vary significantly (
DOMAIN 3. ISSUES OF INTER-CLINICAL AGREEMENT (ARISING FROM UNCLEAR RULES/REGULATIONS):
The 2 groups of respondents mostly agreed that a lack of clarity regarding clinic responsibilities and authority was the source of some ethical issues, as certain clinics would avoid responsibility for their patients, referring those not suitable for tertiary ICU treatment to other ICU departments (
There was also a significant difference of opinion between the 2 groups (
DOMAIN 4. FUTILE TREATMENT:
The respondents held dissimilar views regarding the insistence of both physicians and patients’ relatives on continuing futile treatment, with surgical residents noting such instances to be more frequent compared to internal medicine residents (
However, there was no significant difference between the 2 groups with respect to the prevalence of ICU ethical issues such as conducting constant examinations of and providing unhelpful treatment to patients with minimal signs of life (
DOMAIN 5. PATIENTS’ RELATIVES CREATE ETHICAL ISSUES:
The respondents indicated that the verbal or physical intervention of patients’ relatives, whether directly or through other authorized persons, creates ethical problems. The views of the internal medicine residents and surgical residents did not significantly differ on this point (
DOMAIN 6. INTRA- AND INTER-CLINICAL ETHICAL PROBLEMS:
Most members of the 2 groups agreed that major ethical issues do not frequently arise as a result of professors’ different treatment methods/models, the residents’ own inexperience, and lack of intra-clinical communication (
However, internal medicine residents were more likely to respond that some ethical issues are triggered by stress/anxiety on the part of patients’ relatives, together with residents’ difficulties in discussing informed consent (
DOMAIN 7. RESIDENT HIERARCHIES CREATE BARRIERS:
Regarding the statement that ethical problems in the ICU occurred as a result of the residents’ lack of authority, the views of the 2 groups diverged significantly, with surgical residents less likely to agree (
There were no significant differences between the 2 groups, however, with respect to the proposition that residents should not be actively involved in solving ethical problems in the ICU; both groups also reported similar levels of being the sole individual tasked with resolving ethical issues they encountered in the ICU (
DOMAIN 8. SUGGESTIONS TO RESOLVE ETHICAL ISSUES:
The respondents suggested necessary precautions to help resolve ethical issues arising in the ICU, including improving intra- and inter-clinical communication, the establishment of hospital ethics committees and consultations with medical ethicists, more careful management of supplies and equipment in ICUs to prevent shortages, and ethics training for ICU staff. There were no significant differences between the views of the 2 groups on any of these points (
Discussion
ICU medical residents who work full-time in critical care face the same types of ethical problems as other healthcare workers in the admission of patients, medical decision-making and treatment, and discharge processes, which demand values-based attitudes, behaviors, and actions. Resolving issues related to patient admission, treatment, and discharge will contribute to providing more effective healthcare services.
The ethical issues represented by the 8 domains herein have also been identified in several studies conducted by nurses and physicians in various countries [6–8]. Previous studies have suggested that to resolve the problems in the first domain, it is necessary to ensure that the process of ICU patient admission and discharge is in accordance with medical criteria and involves inter-clinical cooperation and clear communication [8,9]. This approach will help guarantee that the time allocated to the patient within the ICU is used most effectively, thus avoiding ethical issues and allowing the patient to receive proper treatment, from both a medical and ethical standpoint [9].
The issue of scarcity of resources negatively affects ICU patient admission, morbidity, and mortality. Studies on this topic have emphasized the importance of the scarcity of resources and medical staff on ICU outcomes, revealing the disruptions caused to ICU services and the harm incurred by patients, especially during a pandemic [9,11]. Since inadequate resources and staff contributes to ICU employee dissatisfaction, burnout [10], and feelings of helplessness, these may lead to conflicts among those employees and between the latter and hospital management, thus affecting the quality of health services in the ICU.
Regarding ICU administration, the issue of providing information and training on business and management ethical codes for hospital and clinic managers has not yet been seriously discussed. To that end, written guidelines should be prepared to outline protocols for ICU practices according to the job description [12]. Such protocols would help guide collaborations between specialists for critically ill patients, establish guidelines for dealing with anxious or angry relatives of patients, and clarify hierarchies of healthcare professionals, both intra- and inter-clinic, with the aim of eliminating discrepancies in how ethical issues are resolved [13]. Health authorities should also incorporate fundamental principles of accountability and mutually respectful and collaborative relationships to provide better ICU service [14].
Although numerous studies have critiqued the practice of futile or inappropriate treatment, this subject remains under discussion and possible solutions have yet to be implemented [15]. Some physicians do not condone the insistence on treating patients with severe irreversible damage or those who cannot live outside of an intensive care setting, noting that such treatment strains resources, thus causing financial damage [16], and is a waste of time/labor, resulting in other patients being denied ICU access while also dismaying healthcare professionals and patients’ families [17].
Although the context of the present study was quite limited, the respondents noted that it was not uncommon that in the course of visiting a patient, some relatives and even neighbors would attempt to intervene in their treatment. Previous studies have revealed the extent of violence against health professionals [18,19]. A study conducted in Turkey found that in cases of violence committed against healthcare professionals, the perpetrators were overwhelmingly relatives of patients, 95.1% being male relatives [18]. Although the patient-caregiver-family triad contributes to humanizing the caregiving process for the patient and to building better communication and relationships among the members of the triad [20], the stress experienced by the family/relatives may also disturb the caregiver, both due to the possibility of infection and by increasing the stress levels of the latter, potentially leading to burnout. Relatives of patients often report discomfort with the approach of healthcare professionals [21]; such complaints indicate the dissatisfaction felt by both sides. Therefore, ICUs require a novel strategy and training program to handle issues involving patients and their relatives/visitors [22] to improve the safety of both patients and healthcare workers [22]. These guidelines, to be clearly explained to all ICU visitors, should encompass ICU rules such as appropriate distancing, the maximum number of visitors allowed, visiting hours, and hygiene.
Intra-team ethical conflicts may occur due to poor communication, lack of understanding of one’s responsibilities/duties in setting treatment goals, or disagreement regarding ethical judgments, ICU resources, or limitations of the clinics in terms of their tasks [23]. To resolve these kinds of issues, clinic and hospital managers should determine the criteria necessary to positively influence the ICU staff and contribute to their health professional skills so they acquire the ability to resolve ethical issues and provide ethical care. The basic factors leading to poor outcomes in ethical ICU care are poor communication and poor relationships (both among staff as well as between staff and patients/patient relatives) [23], hierarchy problems [24], lack of trust, limited time and resources [25], and interpersonal, intra-clinic, or inter-clinic conflicts [11,13]. These issues may result in delays in implementing necessary ethical interventions, ultimately rendering the problem possibly unsolvable if left too long.
Apart from their low position in the ICU hierarchy and hence relative lack of authority, residents also lack experience compared to the other ICU physicians, yet nonetheless may be left to resolve ethical problems on their own. Although studies have found that there may be barriers to residents’ completing their programs and incorporating new skills in the ICU [26], they can overcome these obstacles and successfully advance their clinical practice with a reevaluation of these programs. Relevant studies have concluded that residents’ main problems stem from the inability to find a mentor, dyssynchronous perspectives between the residents and program leaders, unequal research opportunities [27], and uncertainty with respect to their programs [28]. Other researchers have recommended ethics courses for residents [27]. While the latter may participate in ICU decision-making concerning ethical issues, they nonetheless feel unable to share their thoughts and make possible suggestions [24].
Previous research has suggested resolving ethical issues in the ICU by clarifying intra- and inter-clinical roles and responsibilities, monitoring resources more closely, improving communication with patients and their relatives, establishing hospital ethics committees and consulting clinical ethics specialists, and offering ethics training for all ICU staff [14]. Nearly all studies regarding ethical issues stated that the main problems stemmed from poor communication, lack of good relationships, scarcity of resources, and inter-and intra-clinical conflicts.
Conclusions
This is the first study in Turkey in which ICU medical residents expounded on the ethical problems they face in their daily clinical practice. Our findings support those of previous studies related to ICU clinical ethics issues in the 8 primary domains investigated.
Ethical issues in the ICU do not end with obtaining informed consent, because medical ethical principles such as beneficence, non-maleficence, respect for patient autonomy, and distributive justice also apply, beginning with hospital admission until the patient is discharged. Therefore, it is critical to identify all possible ethical problems that may be encountered and to produce solutions. Ethical issues are not solely the responsibility of the chief clinician, but concern all members of the ICU team involved in patient treatment as well as hospital management.
This study revealed the importance of seeking and comparing the views of all ICU residents on the ethical problems they encounter, understanding the challenges faced by all ICU employees (some of which may become ethical issues), and identifying the factors involved, to find solutions. Our findings suggested that ethics courses for residents, reevaluation of their position in the ICU hierarchy, the establishment of clear guidelines on ethical issues (in written format), and collaboration with other ICU staff represent the most effective methods for handling these challenges.
Limitations
We acknowledge the fact that our study was conducted with a relatively small sample size, but nevertheless believe these findings will be relevant to the majority of programs that seek to improve understanding of residents’ views on ethical issues. ICU residents already maintain a very busy work schedule, while the scarcity of time, the drive for efficiency, and the focus on technology in ICUs, together with the COVID-19 pandemic, have all made this profession much riskier and the workload heavier; as a result, the willingness of ICU residents to participate in research has drastically decreased. A strength of this study is fact that our findings are consistent with the results of other studies on ICU ethical issues, indicating that the present study was well designed and produced results that merit consideration. In addition, few studies have explored the perspectives and experiences of ICU residents; therefore, we believe it represents a worthy contribution to this field.
References
1. Pavlish CL, Brown-Saltzman K, Raho JA, Chen B, A national survey on moral obligations in critical care: Am J Crit Care, 2019; 28(3); 183-92
2. El Jawiche R, Hallit S, Tarabey L, Abou-Mrad F, Withholding and withdrawal of life-sustaining treatments in intensive care units in Lebanon: A cross-sectional survey of intensivists and interviews of professional societies, legal and religious leaders: BMC Med Ethics, 2020; 21(1); 80
3. Akdeniz M, Yardımcı B, Kavukcu E, Ethical considerations at the end-of-life care: SAGE open Med, 2021; 9 20503121211000918
4. Power N, Plummer NR, Baldwin J, Intensive care decision-making: Identifying the challenges and generating solutions to improve inter-specialty referrals to critical care: J Intensive Care Soc, 2018; 19(4); 287-98
5. Chamsi-Pasha H, Chamsi-Pasha M, Albar MA, Ethical dilemmas in the era of COVID-19: Avicenna J Med, 2020; 10(3); 102-5
6. Pishgooie AH, Barkhordari-Sharifabad M, Atashzadeh-Shoorideh F, Falcó-Pegueroles A, Ethical conflict among nurses working in the intensive care units: Nurs Ethics, 2019; 26(7–8); 2225-38
7. Park DW, Moon JY, Ku EY, Ethical issues recognized by critical care nurses in the intensive care units of a tertiary hospital during two separate periods: J Korean Med Sci, 2015; 30(4); 495-501
8. Van den Bulcke B, Metaxa V, Reyners AK, Ethical climate and intention to leave among critical care clinicians: An observational study in 68 intensive care units across Europe and the United States: Intensive Care Med, 2020; 46(1); 46-56
9. Rigaud JP, Giabicani M, Beuzelin M, Ethical aspects of admission or non-admission to the intensive care unit: Ann Transl Med, 2017; 5(Suppl 4); S38
10. Santhosh L, Brown W, Ferreira J, Practical tips for ICU bedside teaching: Chest, 2018; 154(4); 760-65
11. Doyle S, Sharp M, Winter G, Twelve tips for teaching in the ICU: Med Teach, 2021; 43(9); 1005-9
12. McGuire A, McConnell PC, Resource allocation in ICU: Ethical considerations: Curr Opin Anaesthesiol, 2019; 32(2); 190-94
13. Utami PS, Asmaroini AP, Cahyono H, Pelatihan Pemanfaatan Program Mendeley Dekstop dalam Pembuatan Citasi Karya Ilmiah bagi Mahasiswa di Kabupaten Ponorogo: J Pengabdi Masy Darma Bakti Teuku Umar, 2021; 2; 2
14. Sunstein CR, Thaler RH, No title: Univ Chicago Law Rev, 2003; 70; 1159
15. Rose L, Interprofessional collaboration in the ICU: How to define?: Nurs Crit Care, 2011; 16(1); 5-10
16. Prior SJ, Mather C, Miller A, Campbell S, An academic perspective of participation in healthcare redesign: Health Res Policy Syst, 2019; 17(1); 87
17. Kon AA, Shepard EK, Sederstrom NO, Defining futile and potentially inappropriate interventions: A policy statement from the Society of Critical Care Medicine Ethics Committee: Crit Care Med, 2016; 44(9); 1769-74
18. Huynh TN, Kleerup EC, Raj PP, Wenger NS, The opportunity cost of futile treatment in the ICU: Crit Care Med, 2014; 42(9); 1977-82
19. Carter HE, Winch S, Barnett AG, Incidence, duration and cost of futile treatment in end-of-life hospital admissions to three Australian public-sector tertiary hospitals: A retrospective multicentre cohort study: BMJ Open, 2017; 7(10); e017661
20. Sevimli S, An analysis of violence against healthcare professionals in Turkey from online media reports: Eubios J Asian Int Bioeth, 2020; 30(2); 34
21. Quenot JP, Ecarnot F, Meunier-Beillard N, What are the ethical issues in relation to the role of the family in intensive care?: Ann Transl Med, 2017; 5(Suppl 4); S40
22. Opsahl AG, Ebright P, Cangany M, Outcomes of adding patient and family engagement education to fall prevention bundled interventions: J Nurs Care Qual, 2017; 32(3); 252-58
23. Dennis M, Batalini F, Demers L, Upadhyay A, Overcoming barriers to resident scholarly productivity and research at a large academic institution [version 1]: MedEdPublish, 2019; 8; 213
24. Hamui-Sutton A, Vives-Varela T, Gutiérrez-Barreto S, A typology of uncertainty derived from an analysis of critical incidents in medical residents: A mixed methods study: BMC Med Educ, 2015; 15; 198
25. Danjoux Meth N, Lawless B, Hawryluck L, Conflicts in the ICU: Perspectives of administrators and clinicians: Intensive Care Med, 2009; 35(12); 2068-77
26. Nandi PL, Ethical aspects of clinical practice: Arch Surg, 2000; 135(1); 22-25
27. Nadig NR, Sterba KR, Johnson EE, Inter-ICU transfer of patients with ventilator dependent respiratory failure: Qualitative analysis of family and physician perspectives: Patient Educ Couns, 2019; 102(9); 1703-10
28. Celis VI, Méndez CC, Moral distress, sign of ethical issues in the practice of oncology nursing: Literature review: Aquichan, 2019; 19(1); 11-15
In Press
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952